Could a corrective osteotomy be an alternative to the early unilateral knee arthroplasty as gonarthrosis treatment?
The Main task of osteotomy is to postpone initial arthroplasty. Practice witnesses that the later the initial arthroplasty takes place, the lower are chance to need a revision (repeated)
Published: 21.11.2022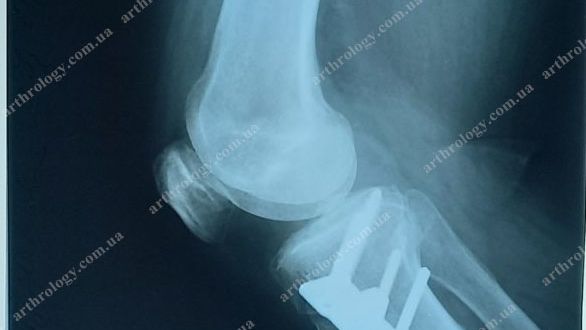
Could a corrective osteotomy be an alternative to the early unilateral knee arthroplasty as gonarthrosis treatment?
The Main task of osteotomy is to postpone initial arthroplasty. Practice witnesses that the later the initial arthroplasty takes place, the lower are chance to need a revision (repeated)
To get more details about gonarthrosis, click “Gonarthrosis – deforming arthritis of a knee”.

An intact joint and gonarthrosis
Facts:
![]() as of 2020, the WHO forecasts that in the next decade, gonarthrosis tends to reach the fourth place as the cause of invalidity in women and the eighth one – in men throughout the world. The question of efficient remedies against gonarthrosis covers medical, social, and economic aspects
as of 2020, the WHO forecasts that in the next decade, gonarthrosis tends to reach the fourth place as the cause of invalidity in women and the eighth one – in men throughout the world. The question of efficient remedies against gonarthrosis covers medical, social, and economic aspects
![]() about 50% of patients with large joints diseases suffer from gonarthrosis
about 50% of patients with large joints diseases suffer from gonarthrosis![]() after the age of 75, about 80% of the population have radiological signs of gonarthrosis, and 30% - both radiological signs and symptoms
after the age of 75, about 80% of the population have radiological signs of gonarthrosis, and 30% - both radiological signs and symptoms![]() in about 85% of cases, gonarthrosis occurs at a workable age, having a significant social and economic impact; in different countries, it causes invalidity in 6.5% to almost 14% of cases
in about 85% of cases, gonarthrosis occurs at a workable age, having a significant social and economic impact; in different countries, it causes invalidity in 6.5% to almost 14% of cases
The causes of the occurrence of gonarthrosis are various and still understudied. Among them, scholars distinguish infections and autoimmune disorders, biomechanical changes of the joint associated with its overload, damage to its components (bones, meniscus, ligaments, capsule), a varus deformity, present in 87% of the gonarthrosis patients and deepening degenerative processes in bony components of a knee.
Corrective osteotomy to tibia and femur as an alternative to early unicondylar knee arthroplasty?

A unicondylar arthroplasty or osteotomy?
The first who documented a high osteotomy as a gonarthrosis remedy was J.P. Jackson in 1958.
During the rapid development in 1960th, this method had split into many types – edge, arch, dome, etc.
Within the development, external ("minus", "closed") and internal ("plus", "open") high tibial osteotomies became the leaders.

The place for corrective tibial osteotomy
Diagnostics, indications, ad benefits of osteotomy
It is extremely important to confirm the diagnosis with diagnostic imaging while planning the treatment.
Diagnostic imaging is the basic instrument to choose the adequate method of treatment – osteotomy of unicondylar arthroplasty
A special plane (Rosenberg or Lyon Schuss plane) allows visualizing the conditions of the damaged portion of the joint. To get it, a patient should stay flexing the knees to 20-30-45 degrees

1. Standing with load 2. Rosenberg / Lyon Schuss plane 3. Standing with knees flexed to 20-30-45 degrees
MRI visualization is more informative

The MRI of a knee for pre-surgical planning
While the X-ray image (on the left) discloses only insignificant subchondral sclerosis and minimal articular gap narrowing, shows no osteophytes and insignificant changes of the patellofemoral joint, the MRI (on the right) demonstrates that almost no cartilage remained in the loaded area of femoral and tibial condyles. There are vivid degenerative changes in menisci, overloaded areas of subchondral bone tissue.
If MRI is unavailable, but there are some reasons to suspect that the X-ray image fails to reflect the whole picture of the pathological changes in joints, a diagnostic arthroscopy is recommended. The direct arthroscopic visualization shows not only the conditions of the cartilage but also other components of the joint – ligaments, menisci, synovial capsule.
Basic criteria and indications for the osteotomy:
![]() 35 or less BMI (relation of body weight to height, calculated individually: body weight (kg) / height2 (m). For example, if body weight = 106 kg, height = 168 cm; hence: BMI = 106 / (1.68 x 1.68) = 37.55 kg/m2)
35 or less BMI (relation of body weight to height, calculated individually: body weight (kg) / height2 (m). For example, if body weight = 106 kg, height = 168 cm; hence: BMI = 106 / (1.68 x 1.68) = 37.55 kg/m2)![]() 1st-2nd stages of deforming knee arthritis, 2nd-3rd stages of insulated arthrosis
1st-2nd stages of deforming knee arthritis, 2nd-3rd stages of insulated arthrosis![]() The absence of patellofemoral arthrosis
The absence of patellofemoral arthrosis![]() Varus or valgus deformity over 15 degrees
Varus or valgus deformity over 15 degrees![]() Range of motions over 100 degrees, complete extension
Range of motions over 100 degrees, complete extension![]() Stable knee joint, intact cruciate ligaments, a normal contralateral component of the joint
Stable knee joint, intact cruciate ligaments, a normal contralateral component of the joint
It is important to remember. According to many authors’ recommendations and observations, no therapeutic manipulations (lavage, debridement, etc.) should be carried out during the arthroscopy at the background of gonarthrosis and incorrect axis of the extremity because they will have no effect. In this case, arthroscopy is the only diagnostic procedure

Criteria of choice for gonarthrosis patients (ISAKOS, 2005)
Absolute contraindications against the osteotomy in gonarthrosis
![]() Rheumatoid arthritis,
Rheumatoid arthritis,![]() 3rd stage of the patellofemoral arthrosis,
3rd stage of the patellofemoral arthrosis,![]() Arthrosis of a joint’s contralateral portion,
Arthrosis of a joint’s contralateral portion,![]() Osteoporosis,
Osteoporosis,![]() Flexion restriction > 25 degrees,
Flexion restriction > 25 degrees,![]() Contralateral meniscectomy,
Contralateral meniscectomy,![]() BMI > 35,
BMI > 35,![]() Lower limbs’ thrombosis,
Lower limbs’ thrombosis,![]() Extraarticular deformities,
Extraarticular deformities,![]() Local and general infections
Local and general infections
A small bone lesion in the area of pathological changes is a relative contraindication, however, such patients have very short-term positive results after the osteotomy
Few words on the benefits of osteotomy
The main advantage of osteotomy is preserving organs. The lack of surgical intervention into the structures of a knee promotes preserving its natural functionality and postponing arthroplasty (joint replacement) to years, and in a case of an adequate conservative treatment – to decades.
According to international studies, after the osteotomy, 8 out of 10 patients can return to sports, habitual way of life, and physical loads. After the osteotomy, the patients have higher activity levels, compared to those after a unicondylar arthroplasty. The survival within 10 years equals 90% (compared to the unicondylar arthroplasty), within 15 years – about 80%, and within 20 years – over 20%.
Advantages and disadvantages of the osteotomy
Advantages:
![]() High accuracy of the correction
High accuracy of the correction![]() High stability with the use of formed tricalcium phosphate blocks
High stability with the use of formed tricalcium phosphate blocks![]() Avoiding shortening of the extremity
Avoiding shortening of the extremity
Disadvantages:
![]() Elongation of the extremity (after a wrong correction)
Elongation of the extremity (after a wrong correction)![]() Less contact with bone tissue
Less contact with bone tissue![]() Durable the bone consolidation
Durable the bone consolidation![]() Patella baja (shortening of the patella’s own ligament)
Patella baja (shortening of the patella’s own ligament)

Pre-surgical planning of osteotomy
1. Clinical examination and establishing indications of the osteotomy
![]() Age of the patient. It is important: a patient's passport age and conditions of joints may not comply with his or her biological age. The patient’s expectations from the operation.
Age of the patient. It is important: a patient's passport age and conditions of joints may not comply with his or her biological age. The patient’s expectations from the operation.![]() Assessing the range of motions of a knee. The presence of flexion-extension contractures, recurvation (knee recurvation (from Latin genu recurvatum) or hyperextension is a pathology specific to an excessive extension of a knee, leading to articular deformities).
Assessing the range of motions of a knee. The presence of flexion-extension contractures, recurvation (knee recurvation (from Latin genu recurvatum) or hyperextension is a pathology specific to an excessive extension of a knee, leading to articular deformities).![]() Assessing gait and functioning of hip and knees while walking.
Assessing gait and functioning of hip and knees while walking.![]() Evaluation of capacities and pathological changes in the knee’s ligament complex (ACL, PCL, MCL, LCL)
Evaluation of capacities and pathological changes in the knee’s ligament complex (ACL, PCL, MCL, LCL)![]() Examination of the skin – scars, inflammations, knee oedema, infection foci
Examination of the skin – scars, inflammations, knee oedema, infection foci

2. Radiological assessment of deformities
![]() Mechanical axis
Mechanical axis![]() SLOP (tibial plateau inclination), especially important for a single reconstructive surgery of knee ligaments – ACL and PCL
SLOP (tibial plateau inclination), especially important for a single reconstructive surgery of knee ligaments – ACL and PCL![]() Joint line
Joint line![]() Location of the deformity
Location of the deformity![]() Position and tracking of the patella
Position and tracking of the patella
3. The correlation between the clinical and radiological conditions
4. Planning of the correlation
5. Choosing an implant
6. Choosing a material for the replacement in a case of open osteotomy
7. Availability of a computer-aided navigation
8. Arthroscopy is the first stage of any osteotomy around the knee
Complex deformities may demand two-level osteotomies involving the tibia and femur to recover full-range biomechanics and joint line


1. Axial Rg (Merchant’s plane) 2. Finding the Caton-Deschamps index (normal value - 1:1+/-20%) 3. Calculation by Coventry 4. Calculation by Maniatsi. Correlation between clinical and radiological conditions, planning the desired correlation
Choosing an implant for the osteotomy

Today, there is a vast variety of osteotomy fixations. The main requirements are stable fixation and minimal irritation to soft tissues.
![]() Autograft bone has the lowest risk, however, its collecting causes additional trauma to the patient's tissues and increases the duration of the surgery and anaesthesia.
Autograft bone has the lowest risk, however, its collecting causes additional trauma to the patient's tissues and increases the duration of the surgery and anaesthesia.![]() Allobone allows for avoiding additional trauma. However, according to some authors, this type of bone graft most frequently leads to nonunions in the area of correction, plus it bears some moral aspects.
Allobone allows for avoiding additional trauma. However, according to some authors, this type of bone graft most frequently leads to nonunions in the area of correction, plus it bears some moral aspects.![]() Tricalcium phosphate blocks do not require additional traumas, are available, highly stable, allow adjustment of the desired shape and angle of the correction in advance.
Tricalcium phosphate blocks do not require additional traumas, are available, highly stable, allow adjustment of the desired shape and angle of the correction in advance.
Computer-aided navigation helps to perform the operation correctly and place an extremity's axis into the planned position. However, one shouldn't rely on the computer's aid completely because those doing such surgeries without adequate experience could make mistakes.
Arthroscopy as the first stage of any osteotomy is a necessary manipulation in today's practice. It serves for visual assessment of external and internal knee joint, and tissues of the patellofemoral one. It also enables the removal of small damages to the menisci and micro-perforation of the knee's tibial and femoral components.

Tibial and femoral osteotomies
Assessing the results of osteotomy
A correctly planned and performed osteotomy is beneficial for a knee joint.
After the union, approximately a year and a half, the fixing device has to be removed. It is the right time for a visual assessment of the structures of the knee, especially the tibial and femoral cartilage
To evaluate regeneration of the cartilage, doctor Koshino T. et al. in 2003 developed a scale, where:
![]() Stage А means no regeneration of the cartilage
Stage А means no regeneration of the cartilage![]() Stage В means partial regeneration of the fibrosis-cartilage tissue
Stage В means partial regeneration of the fibrosis-cartilage tissue![]() Stage C means a completed closure of the cartilage defect with an uneven (tuberous) fibrosis-cartilage tissue (C1) and smooth cartilage (C2)
Stage C means a completed closure of the cartilage defect with an uneven (tuberous) fibrosis-cartilage tissue (C1) and smooth cartilage (C2)

Classification of cartilage regeneration by Koshino. Stage А: no regeneration; stage В: partial regeneration of fibrosis-cartilage tissues; stage С: the lesion gets completely closed with an uneven (tuberose) fibrosis-cartilage tissue (C1) and smooth cartilage (C2). 1. Stage B. 2. Stage C
The images below illustrate the result of the recovery of cartilage depending on the angles of correction to valgus deformity eighteen months after the osteotomy. The observations evidence that the correction of a valgus 3 degrees and over have a positive result (B, C1 and C2 according to the Koshino scale) more than in 90% of cases. We treat this as a very positive result and an alternative to a unicondylar arthroplasty for young patients. Except for cartilage recovery, recovery of functions and the range of motions is vivid, pain decreases significantly.


- Group 1: 10 patients, varus correction angle from 3 to 0 degrees
- Group 2: 25 patients, valgus correction angle from 1 to 3 degrees
- Group 3: 15 patients, valgus correction angle over 3 degrees
Correlation angles and results
Example of osteotomy results
A male 52-years-old patient with a 5 degrees varus deformity, medial osteoarthritis underwent corrective osteotomy of about 2 degrees. Conditions before the surgery and eighteen months thereafter
Before the surgery:
![]() KOOS - 60
KOOS - 60![]() KSS - 70
KSS - 70![]() VAS - 7
VAS - 7
After the surgery:
![]() KOOS - 86
KOOS - 86![]() KSS - 95
KSS - 95![]() VAS - 1
VAS - 1

Arthroscopy results: The medial portion after 18 months: stage B by Koshino; lateral portion: stage C by Koshino

1. Medial portion of the joint: a) initial arthroscopy, b) in 18 months 2. The lateral portion of the joint: a) initial arthroscopy, b) in 18 months
A Swedish register for 1998-2007 provides a generalized result of corrective osteotomies (3161 surgeries) and subsequent total knee arthroplasties

TNA after corrective osteotomies (according to the Swedish register)
The researchers note that X-ray visualizations within the observation period demonstrate the absence of any signs of progressing gonarthrosis; in rare cases, it discovers a slight worsening of a joint's contralateral portion's conditions.
The analysis involved results of studies of the use of TKA after a corrective osteotomy. Some publications declare the complexity of arthroplasties (joint replacements) after corrective osteotomies, noting the increase in the share of complications to 30%. However, the majority of orthopaedic surgeons share the idea that after a correctly calculated osteotomy, initial arthroplasties don’t have any technical peculiarities. Moreover, implanting an endoprosthesis into an anatomically normal knee shows better long-term results.
To sum up this brief review, we would like to emphasize the following:
Osteotomy demonstrates positive results on gonarthrosis up to the 3rd stage thereof, confirmed many times in numerous pieces of research and long-time observations. Correct and accurately following indications, the choice of implants ensures positive long-term results. However, the duration of the effect and positive influence of the corrected axis on the joint depends not only on a surgeon's expertise and virtuosity of surgery. Good outcomes demand a large extent of a patient's contribution. To fix the result and postpone the need for arthroplasty, and, as the best variant – to be able to avoid the joint replacement, it is needed:
![]() reducing weight to physiologically optimal values, applying diets, sports, yoga, metabolism correction, strengthening the muscles of the shin and thigh to stabilize the axis of the extremity;
reducing weight to physiologically optimal values, applying diets, sports, yoga, metabolism correction, strengthening the muscles of the shin and thigh to stabilize the axis of the extremity;![]() use custom-made orthopaedic insoles to recover biomechanical features of the ankle and the whole leg;
use custom-made orthopaedic insoles to recover biomechanical features of the ankle and the whole leg;![]() take medications: except for contraindication cases, hyaluronic acid, PRP, and other regenerative therapies enhance the regeneration of the tissues of the joint;
take medications: except for contraindication cases, hyaluronic acid, PRP, and other regenerative therapies enhance the regeneration of the tissues of the joint;![]() attend your orthopaedic surgeon at least once a year to control the conditions of the joint.
attend your orthopaedic surgeon at least once a year to control the conditions of the joint.
Thus, the purpose of the corrective osteotomy is the normalization of knee biomechanics to suspend the development of arthrosis; it could be done, if the arthrosis has damaged only one condyle, and up to its 3rd stage.
A unicondylar arthroplasty takes place if the arthrosis of a condyle of a knee reaches the 3rd stage of development.
We can conclude that osteotomy is not an alternative to a unicondylar knee arthroplasty. Each of the methods has indications and contraindications.
And as we always do, we'd recommend the patients not to use self-treatment with "folk" remedies! This is especially important in the case of gonarthrosis. There are no folk remedies able to stop its progression. And while initial stages are curable for conservative treatment plus osteotomy, only total knee arthroplasty can recover the joint’s mobility and get rid of pain at the 3rd and 4th stages



- Tag:
- Osteotomy
- corrective osteotomy
- alternative to joint replacements
- gonarthrosis
- knee osteoarthrosis
- knee arthroplasty
- unicondylar arthroplasty